Leaky gut has become a household term. However, while it’s easy to find information online, in books, through courses, and even in pamphlets at your doctor’s office, leaky gut myths abound.
Many patients continue to suffer or feel frustrated due to widespread misinformation on the causes and solutions for leaky gut syndrome.
In this article I will introduce you to the top five leaky gut myths and misunderstandings.
Tight junctions and leaky gut
First, it’s helpful to understand a bit about the gut wall. The intestinal walls consist of cellular “tight junctions.” These act as a protective barrier that selectively allow nutrients into the bloodstream while preventing the entry of pathogens and other unwanted compounds that can trigger inflammation.
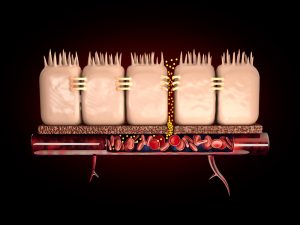 Leaky gut — known as “intestinal permeability” in the scientific literature — occurs when the gaps of the tight junctions widen and allow larger particles to pass into the blood stream. This triggers an immune cascade that results in systemic inflammation and increases the risk for food sensitivities, pain, autoimmune disease, and other health problems.
Leaky gut — known as “intestinal permeability” in the scientific literature — occurs when the gaps of the tight junctions widen and allow larger particles to pass into the blood stream. This triggers an immune cascade that results in systemic inflammation and increases the risk for food sensitivities, pain, autoimmune disease, and other health problems.
The damage doesn’t stop there. The same factors that lead to leaky gut also lead to “leaky brain” in which the blood-brain barrier, a protective membrane surrounding the brain, becomes over-permeable and allows pathogens to enter the brain. This creates brain inflammation.
For many people leaky gut and leaky brain go together. What’s more, without a properly functioning brain, your gut can’t function well either.
Leaky gut myth #1: There is no research on leaky gut
Typically, the term “leaky gut” is not used in scientific papers. Instead, researchers most often use the term “intestinal permeability.” A search of the National Library of Medicine (pubmed.gov) database pulled up nearly 5330 papers with the term “intestinal permeability” in the title or abstract.
This is why doctors will say leaky gut is a myth when patients ask about it.
However, a drug for leaky gut is currently being clinically trialed and a recent pubmed.gov search found 418 peer-reviewed papers using leaky gut in the title or abstract.
The awareness of leaky gut will continue to rise along with the growing body of research linking it to autoimmunity, mood disorders, diabetes, and many other common health disorders.
Leaky gut myth #2: You can fix leaky gut with nutritional supplements
Maybe, maybe not. Leaky gut is not a nutritional deficiency and assuming a nutritional supplement will fix it is illogical.
Instead, you have to ask, “What causes intestinal permeability?” Many factors can play into leaky gut, such as hormone deficiencies, inflammation, autoimmune disease, food sensitivities, and more.
It is when we can identify the underlying factors unique to each patient that we can begin to make true progress.
Supplements and botanicals commonly used to support leaky gut include short-chain fatty acids (such as butyrate), glutamine, and marshmallow extract. These all have anti-inflammatory effects on the gut, but they do not address the underlying trigger.
There is NO one-size-fits-all leaky gut solution: If you search, you’ll undoubtedly find variations on a “leaky gut protocol” of specific supplements or protocols — recommended for everyone regardless what their unique underlying factors are.
While they may help, you need to dial in on the underlying mechanisms to genuinely address leaky gut.
And, while some underlying mechanisms behind leaky gut can be fixed, some cannot. For example, autoimmunity can contribute to leaky gut on a cyclical basis. As the autoimmune-based inflammation comes and goes, the tight junctions in the gut wall can repeatedly become leaky and symptoms will arise again.
Or, someone who has chronic prediabetes and high levels of HbA1c may have repeated breakdowns of the tight junctions which lead to ongoing leaky gut.
In these cases, managing leaky gut will likely be a life-long project. Supplements can help, but they are not going to address the root cause.
Is it hopeless? No. In functional medicine we see that about 20 percent of leaky gut patients can be helped solely with supplementation.
For the remaining 80 percent, it’s necessary to home in on the underlying mechanisms before you can really make an impact.
 Leaky gut myth #3: If you have multiple food sensitivities, you must also have leaky gut
Leaky gut myth #3: If you have multiple food sensitivities, you must also have leaky gut
Having multiple food sensitivities is not always associated with leaky gut. In fact, many patients who do not have leaky gut who have chronic food sensitivities.
At the root of food sensitivities is what we call loss of oral tolerance. Oral tolerance is the body’s ability to properly recognize and respond to food proteins.
When we lose oral tolerance, our immune system overreacts to dietary proteins and treats them as if they are foreign invaders. Intestinal permeability can be involved, but other factors include overactive dendritic cells, dysfunctional regulatory T-cells, and over reactive Kupffer cells in the liver.
Loss of oral tolerance is very common with chronic illness and autoimmunity, and is the foundation of food sensitivities.
You can learn more about loss of oral tolerance here.
Leaky gut myth #4: If you fix your leaky gut, you will get rid of your food sensitivities
Maybe: A patient has leaky gut from a highly inflammatory diet or chronic antibiotic use. Their tight junctions break down, and now they have leaky gut.
They take supplements, clean up their diet, and reduce their chronic stress. As a result, their tight junctions recover and their symptoms improve.
Maybe not: Many people have more complicated mechanisms behind their leaky gut. One such case would be celiac disease, in which a lifelong immune reactivity to gluten has significantly damaged the gut wall.
Another patient has cross-reactivity to a food such as to nightshades — when they eat this food their immune system attacks tissue in their body that contains identical amino acid sequences. This will occur regardless of the status of their gut wall.
For these patients, addressing leaky gut can improve their gut health, but it will not eliminate the cross-reactivity or celiac disease.
Leaky gut myth #5: Autoimmune diseases are caused by leaky gut, so fixing leaky gut will cure the autoimmune disease
Autoimmune diseases are not curable. But it is possible for some autoimmune patients to put their symptoms into remission with the proper protocols.
However, as anyone with autoimmunity knows, various things can trigger a flare up. These include stress, toxins, viral infections, inflammation, food reactivity, and other factors.
These autoimmune flares can also trigger leaky gut.
On the flip side, how aggressive the autoimmune disease is and how often it flares up can be impacted by the health of the gut.
If you can reduce your exposure to inflammatory dietary and lifestyle factors, repair the gut, and reduce your general inflammation, it may help you go into remission again.
For many autoimmune patients, living well with autoimmunity means constant management of the factors that cause inflammation.
Now that you know about the top five leaky gut myths and misunderstandings, keep your eye out for my Gut Health course.






I am a 55 female with Hashimotos and in good health all considering although I do feel the cold and deal with anxiety. I do not get colds or flu, I never take pharmaceutical drugs and try to carefully away from unnecessary toxins. I exercise every day, am not overweight, and follow the autoimmune protocol. I am being pressured into having the covid vaccine by my family. When I came to the UK the usual thyroid tablet I was taking in conjunction with a natural thyroid hormone was not available and was asked to try another one. After just the second tablet, I felt really ill, fatigued, flu-like aches, and joint pain, nausea. I reacted, in the same way, I would gluten. I also react to wood varnish in the same way and am highly sensitive to smoke, perfume, and the cold. With the vaccine being a cocktail of ingredients, some of which are synthetic, I am concerned I may react to one of them and that it makes me really ill, and then I have no way of knowing how long if I do react, the debilitating symptoms will take to wear off. I was advised by a Dr in South Africa not to take the HRT in the UK as it was synthetic and might cause an autoimmune flare-up. In light of the risks of covid, where only 1% of the population have died of this virus, the average age being 83, I believe I am better not to have the vaccine, but what would you advise?